The first recorded outbreak of Ebola virus disease began on June 27, 1976, in Sudan, and simultaneously in Zaire (now the Democratic Republic of Congo). These dual outbreaks introduced the global community to a new and terrifying pathogen—one that caused rapid deterioration, internal bleeding, and death in a high percentage of those infected. The emergence of Ebola forced the world to reckon with the threat of viral hemorrhagic fevers and highlighted the vulnerabilities in global health systems.
A Deadly Discovery
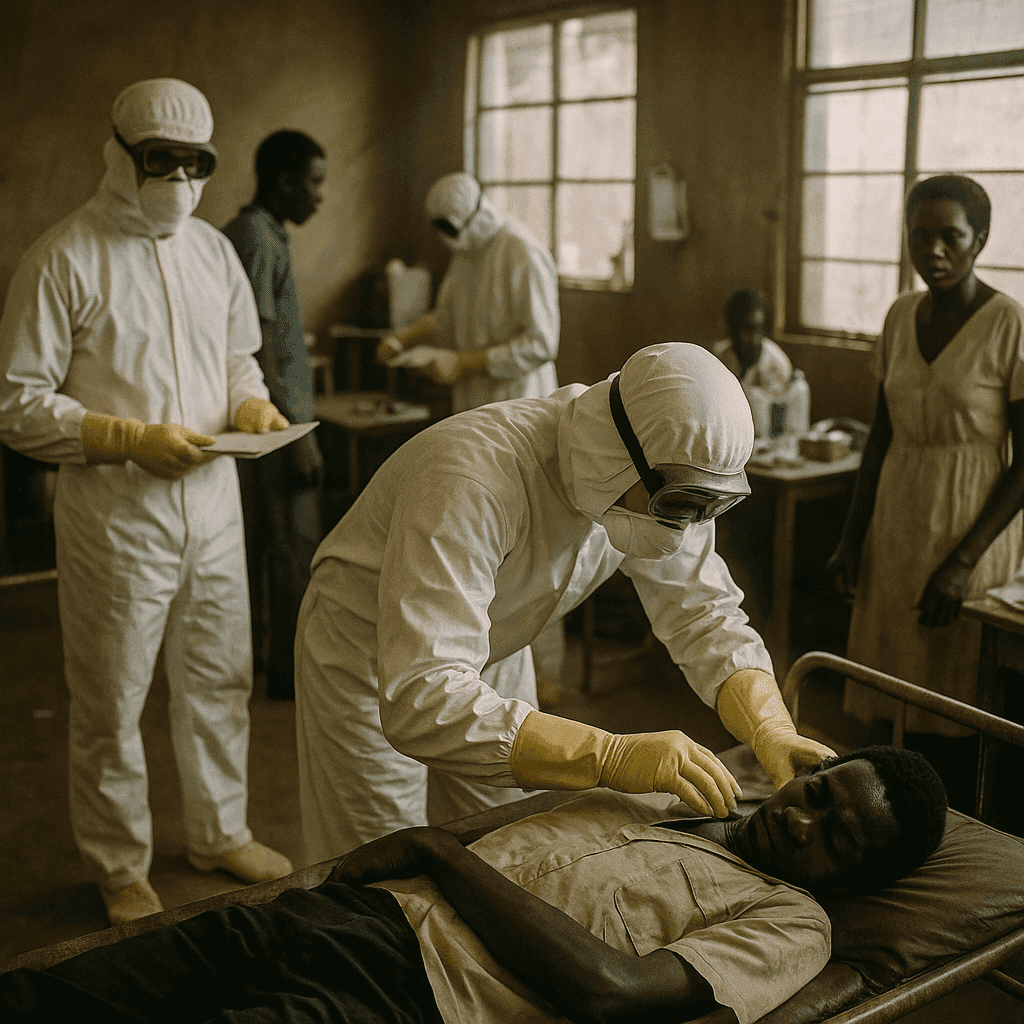
The 1976 outbreak in Sudan began in the town of Nzara, where textile factory workers started falling ill with fever, vomiting, and bleeding. Health officials were alarmed not only by the severity of the symptoms but also by how quickly the disease seemed to spread. Soon after, a separate but genetically related outbreak struck in northern Zaire, compounding fears that a virulent and poorly understood virus was on the move. In total, more than 600 people were infected during the two outbreaks, with a combined fatality rate of nearly 90 percent in some areas.
Doctors and scientists scrambled to identify the cause of the illness. Blood samples were flown to laboratories in Europe and the United States, where researchers discovered a new filovirus. Named after the Ebola River near the Zaire outbreak, the virus was found to be transmitted through close contact with bodily fluids, posing an extreme risk to caregivers and medical personnel. The discovery would mark one of the most chilling chapters in 20th-century epidemiology.
Global Wake-Up Call

Ebola’s emergence was a sobering reminder that lethal diseases could surface unexpectedly, especially in regions with limited health infrastructure. The outbreaks prompted urgent action from the World Health Organization and other health agencies to improve diagnostic capabilities and outbreak containment strategies. Isolation wards, protective gear, and contact tracing—now standard elements of epidemic response—became central lessons from the 1976 experience.
The lack of effective treatment or vaccine at the time made containment the only viable strategy. The outbreak underscored the need for rapid information sharing and coordination between local and international health authorities. Though it eventually subsided, the outbreak revealed how quickly an infectious disease could devastate communities and overwhelm fragile healthcare systems.
A Legacy of Vigilance and Innovation

In the decades since the 1976 outbreaks, Ebola has re-emerged multiple times, most notably in the 2014–2016 West Africa epidemic, which killed over 11,000 people. Each recurrence has sparked both fear and innovation, driving advances in vaccine development, public health preparedness, and community-based interventions. The approval of the first Ebola vaccine in 2019 was a major milestone in the fight against the virus.
Ebola remains a stark example of zoonotic spillover—diseases that leap from animals to humans—reminding us of the ecological connections that underlie human health. From improved biosafety protocols to global epidemic response teams, much of today’s infectious disease infrastructure can trace its roots to the lessons learned in Sudan and Zaire nearly fifty years ago.